You can lead a horse to water, but you can’t make it drink—this adage is especially true when it comes to implementing predictive analytics in a healthcare setting.
The use of artificial intelligence and machine learning solutions to detect the likelihood of disease is still a hot topic. As anyone who attended this year’s HIMSS conference will tell you, there is no shortage of vendors making grand promises based on what they can do with your data.
However, even the greatest algorithms in the world are of little value, unless they can become actionable and lead to intervention strategies. For example, flagging high-risk patients is only impactful if it leads to actually bringing those patients in for further evaluation or treatment. Otherwise, it is little more than yet another report or measure.
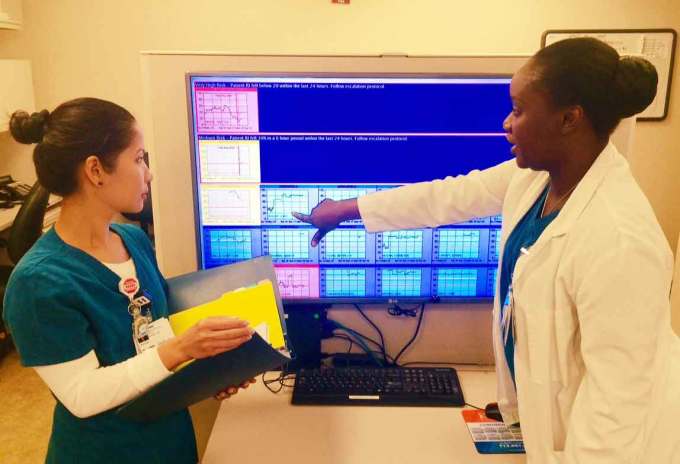
Clinicians at Houston Methodist Hospital review their patients’ Rothman Index scores.
The key issue of workflow is making sure that the data concerning patients flagged at high risk is accepted by those involved—primarily physicians, care managers and case managers—and that they prioritize follow up. The clinical team must consider it imperative to get these patients in for evaluation. Otherwise, there will be skeptics (as with any new technological implementation) arguing from the position of “Why do we need this?”
Concurrently, many clinical and support staff are already bogged down helping patients navigate their care in the health system. These schedulers, or navigators, now must find the resources to take on additional clinical follow-ups and convince patients to visit within a short timeframe.
The key success factor in creating a strong workflow is to make sure that it can create opportunities for timely intervention that can improve patient outcomes by preventing the onset of specific diseases. It’s not just getting the horse to water; we must also get it to drink. However, this entails overcoming a number of challenges:
- Alert fatigue. With average panel sizes of approximately 2,300 patients, primary care physicians are already overworked, with estimates suggesting it would take each doctor 21.7 hours per day to provide all the recommended care for a panel of 2,500 patients. Meanwhile, clinicians are already overwhelmed by the sheer volume of alerts already emanating from EHRs, often having to ignore 49 percent to 96 percent of safety notifications. Now, we are adding additional alerts, which these already-fatigued doctors are expected to notice and prioritize.
- Scheduling. Often understaffed and with lengthy waiting lists for patient follow-up appointments, hospitals will now have to deal with additional lists of people coming in for evaluation. Physicians and care teams must find a way to decide what necessary priority the new, at-risk group receives in relation to the healthcare system’s previously scheduled patients.
- Automation vs. manual administration. Within a clinical workflow, manual steps have been the norm in ensuring that necessary evaluations actually take place: updating flowsheets, taking notes, following up on notifications and insurance checks. Currently, care managers must manually monitor and document all of this in some form of workflow for follow-up appointments and evaluations to be approved. While automation presents the logical answer to these hurdles, this in itself can present concerns. With more automation comes more technology and more intervention by siloed groups. Hospital leaders must therefore find a way to bring together clinicians, care managers, specialists and technical staff in an organization in order to help provide the evaluations indicated for newly flagged at-risk patients.
- Actionable data. Organizations want to solve a multitude of problems with various machine learning and cognitive initiatives, which in turn bring up numerous analytical issues – having to create longitudinal records of all their patients, doing quality scores and ensuring compliance with all the regulatory reporting requirements. For the last several years, these facilities have been integrating big data solutions. However, they have largely failed to produce solutions that help providers with their early detection and prevention of high-burden diseases, as well as facilitating intervention strategies that can reduce risk or prevent onset entirely.
Any new implementation in any industry will not succeed unless there is a culture that embraces innovation and how it can be applied to patient care. This requires leadership that can align the various siloed departments to put forth a solution for the organization. Leadership, and an effective champion who can inspire culture change can help align multiple groups with differing concerns and priorities. Also essential is clear attention to addressing issues relating to risk and responsibility when dealing with confidential or highly sensitive data. Only by bringing them together can an organization be set up for success. Having a champion able to achieve that is essential.
By embracing that shared commitment, organizations can not only improve their quality measures, but demonstrate to their communities that they are being innovative in using new technologies to improve healthcare. This, in turn, can allow them to be more competitive in the market, creating a solution where culture and commitment leads to success.
Another priority is implementing the new solution into current workflows that are already successful, to create a process that doesn’t put extra burden on the organization. Hospital care managers are already reaching out to patients for annual checkups or vaccination programs. Thus, aligning to the current resources that are already successfully bringing patients in and finetuning that message will contribute to success.
Finally, current IT-based clinical initiatives often take many months, or even years, before they even begin to show value. As Eric Topol predicts, “one of the most important potential outgrowths of AI in medicine is the gift of time.” Thus, a truly successful implementation must be one that is disease-specific and able to move extremely fast, driving processes that quickly show value. Only then can success be truly measured. After all, if the results of an implementation do not encompass improved patient outcomes and improved experience of care, it won’t mean a thing.

